CARES Act Healthcare Provider Relief Fund
AAFCPAs would like to make healthcare providers aware that as part of the Coronavirus Aid, Relief and Economic Stimulus (CARES) Act legislation, $100 billion in Provider Relief Funds was pledged to hospitals and other healthcare providers. These funds are designed to reimburse healthcare-related expenses and lost revenue related to COVID-19, and to guarantee uninsured Americans have access to testing and treatment for COVID-19.
On April 10, 2020, the first $30 billion of Provider Relief Funds was infused into the healthcare system via direct deposit to eligible providers. Direct deposit payments were issued by Optum Bank with the note “HHS Payment” in the description. If direct deposit was not previously used with the Center for Medicare and Medicaid Services (CMS), paper checks were mailed and are expected to be received within two weeks. The quick dispersal of funds is meant to provide immediate relief to those healthcare providers heavily impacted by the COVID-19 pandemic.
Who is eligible?
Eligible providers are those who received Medicare fee-for-service (FFS) reimbursements in 2019 (excluding Medicare advantage plans). Payments to providers were determined based on the ratio of the provider’s share of 2019 Medicare FFS reimbursements compared to 2019 total Medicare FFS reimbursements disbursed ($484 billion), multiplied by $30 billion (currently available Provider Relief Funds).
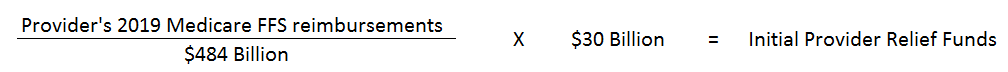
Terms and Conditions
The Provider Relief Funds are considered grants and will not need to be repaid, however, there are certain terms and conditions associated with the grant including:
- Providers who have been allocated a payment from the initial $30 billion general distribution must sign an attestation confirming receipt of the funds and agree to the terms and conditions within 30 days of payment. Please visit the CARES Act Provider Relief Fund Payment Attestation Portal to confirm receipt and accept terms & conditions.
- The provider must have billed Medicare in 2019 and be in good standing with Medicare.
- The provider must be providing testing or care to possible and confirmed COVID-19 patients.
- The funds must be used against qualifying expenses as defined in the grant award and excludes certain expenses related to executive compensation, lobbying expenses, gun control, and more.
- The provider will be subject to various reporting on use of funds and must certify that payments were not used to reimburse expenses or losses already funded by other sources, or obligated to be funded by other sources.
- The provider will be subject to substantiation of expenses or losses incurred as defined and governed by 45 CFR § 75.302 – Financial management and 45 CFR § 75.361 through 75.365 – Record Retention and Access.
- The provider is prohibited from seeking patient out-of-pocket reimbursements over and above what would have been paid in a traditional in-network provider.
Terms and conditions may evolve or be clarified in the next 30 days as required reporting is finalized.
What about the other 70 billion?
The second round of funding is expected to be more targeted towards those providers “who predominantly serve the Medicaid population” in order to ensure care to otherwise un- or under-insured Americans. The expected date of the remaining reimbursements is not yet known. AAFCPAs will monitor communications from the government and keep you informed as changes occur.
How may we help?
AAFCPAs is available to assist clients in answering questions you may have on eligibility and use of funds, and to provide guidance on tracking and monitoring of expended funds in accordance with the regulations.
CARES Act/COVID-19 Task Force
AAFCPAs’ CARES Act Task Force is dedicated to studying and advising clients on the business implications of the Coronavirus Aid, Relief and Economic Stimulus (CARES) Act legislation, signed by President Trump on Friday, March 27th, 2020. Our CARES Task Force includes senior leadership and advisors from diverse segments of our organization—including our Healthcare practice—bringing the necessary talent together to best advise on the changing dynamics caused by the Coronavirus. Learn more. >>
If you have any questions, please contact Courtney McFarland, CPA, MSA at 774.512.4051, cmcfarland@nullaafcpa.com; or your AAFCPAs Partner.

