Denials Management: Best Practices in Improving Revenue Cycle Processes & Monitoring Third-Party Payer Denials
 The complexities surrounding third-party revenue cycle management, patient eligibility, and systems capabilities to support process design changes continue to increase, as do third-party claim denials across virtually all payers. Denials can affect the bottom line of healthcare organizations, leading to lost revenue and productivity; however, in many cases, denials are preventable. In order to prevent denials, it is critical that healthcare organizations develop & implement an effective denials management process, including: strong controls & processes at all stages of the revenue cycle; active monitoring to understand the nature & cause of ongoing denials; and an ongoing commitment of continuous improvement to prevent denials, and improve collections. AAFCPAs provides the following best practices, and key denials management principles and techniques to guide our clients who are healthcare providers in developing and institutionalizing a denials management process.
The complexities surrounding third-party revenue cycle management, patient eligibility, and systems capabilities to support process design changes continue to increase, as do third-party claim denials across virtually all payers. Denials can affect the bottom line of healthcare organizations, leading to lost revenue and productivity; however, in many cases, denials are preventable. In order to prevent denials, it is critical that healthcare organizations develop & implement an effective denials management process, including: strong controls & processes at all stages of the revenue cycle; active monitoring to understand the nature & cause of ongoing denials; and an ongoing commitment of continuous improvement to prevent denials, and improve collections. AAFCPAs provides the following best practices, and key denials management principles and techniques to guide our clients who are healthcare providers in developing and institutionalizing a denials management process.
Preventative Measures Over Denials in the Revenue Cycle
An effective denials management process follows the entire revenue cycle from beginning to end.
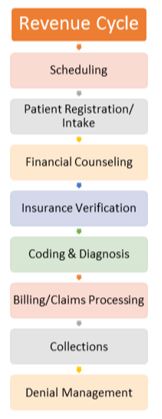
AAFCPAs believes that it is crucial for organizations to dedicate sufficient resources at the beginning of the revenue cycle, including: front-desk staff training, financial counselors and effective insurance verification. These resources and processes should be complemented with a strong cash-collection process over co-pays and nominal charges. AAFCPAs encourages clients to actively monitor the ratio of point-of-service cash collections to total cash collections. Organizations that maximize patient-portion collections at registration minimize collection costs post-encounter, and improve this critical key performance indicator.
After an encounter has taken place, and the billing and collection responsibilities have transferred to coders and billers, providers should apply a claims check or “scrubbing” process that allows for billers to identify potential denials before they are submitted to insurers. Effective claims scrubbing processes are far less costly than re-billing and chasing an already denied claim.
At the back-end of the revenue cycle there are a myriad of controls and processes that should be in place to monitor, track and follow-up on third-party payer denials. Effective denial management is only as strong as the resources dedicated to the process. Practice management systems capabilities may need to be reviewed to ensure your organization is effectively tracking the necessary denial data. Further, the system must be capable of producing meaningful reporting to support improvements.
Once the nature and extent of denials is reportable, management may begin to analyze and correct claims for resubmission. AAFCPAs encourages clients to focus on the “low hanging fruit” initially to improve collections. Immediate attention should be given to claims that are preventable in nature. Once a proper denial reporting process is in place, systematic issues resulting in repeat denials should become apparent relatively quickly. Common preventable claims include: letting payer billing deadlines lapse, provider credentialing issues, patient eligibility issues, coding errors, and prior referral / authorization documentation, among others.
In order for denial management to be effective, organizations must commit to dedicate specific billing personnel and other resources to regularly monitor, report and re-bill denied claims. This team should have a mindset and clear expectation of continuous process improvement to remedy preventable denials at the onset of the encounter.
Implementing Key Performance Indicators (KPIs) over Denials
After organizations have implemented preventative measures over denials to the revenue cycle, the next step is implementation of regular reporting and management. Depending on service type, programs, and nature of the organization, healthcare entities should identify the key performance indicators over denials that are most critical to identifying trends and ensuring billing and collections are operating as effectively as possible. Some common KPIs for denial management include: collection ratios, denial write-off ratio, denial re-submission collection rate, and clean claims submission rate. Implementing KPIs over denials to monthly financial reporting will help set goals and expectations to further define success over the third-party billing processes.
Understanding Denial Causes
The need for a robust denial management process should be clear. As healthcare organizations continue to merge, take on alternative payment contracts, expand and diversify services, it is ever more important to delineate the causes and sources of denials. Based on certain payer-specific requirements, or community program requirements, some denials are inevitable. Denials should be tracked and reported for program accomplishment and statistical purposes, and classified as preventable versus non-preventable. Some of the most common issues that come to light after denials have been effectively reported and summarized are often isolated in nature. For example, healthcare organizations may find that one single provider site is an outlier causing more denials, and that these are due to front desk control breakdowns specific to that site. Given the rate of provider turnover in the healthcare industry in recent years, it is not uncommon to learn that a significant amount of denials are related to delays or errors in credentialing new providers. Additionally, a thorough analysis of denials will identify issues with specific payers and will give billing and collection personnel the opportunity to troubleshoot claims up front with that provider.
AAFCPAs’ Healthcare Consulting & Reimbursement Solutions
This denials management guidance is a fine demonstration of the insights gained by AAFCPAs having spent over four decades providing incisive financial knowledge and strategic management advice to help our clients obtain optimal reimbursements, maintain regulatory compliance, increase cash flow and sustain performance. Our Healthcare Practice, and integrated Business Performance, Internal Controls & IT Advisory Practice provides best practice recommendations and operational process reviews surrounding third-party billing and collection, accounts receivable management, reserve analysis, fee schedule analysis, business process improvement, and recommendations for implementing denial management processes. Additionally, AAFCPAs advises clients in the creation and customization of reports and key performance indicators, so clients are positioned to understand trends and mitigate potential issues relating to their denial management process. We utilize advanced, data extraction software to summarize denial data directly from practice management systems, and convert that data into useful graphs, charts and tables to help management quickly analyze and understand the reasons for denials.
If you have any questions please contact your AAFCPAs partner, or Charlie Webb, CPA at 774.512.4046, cwebb@nullaafcpa.com.

