AAFCPAs supported Boston Senior Home Care in modernizing authorization tracking through intelligent automation, enabling proactive oversight, improved staff efficiency, and meaningful reductions in claim denials.
At a Glance: From Manual PDFs to Proactive Oversight
Managing claim denials depends heavily on accurate, timely authorization tracking, yet many organizations still rely on fragmented manual processes.
Boston Senior Home Care addressed this challenge through intelligent automation, reducing monthly claim denials and transforming a previously manual authorization process that tracked hundreds of PDF approvals each month. This approach improved visibility into expiring and missing authorizations, supported staff efficiency, and shifted authorization management from reactive follow-up to proactive oversight that helps protect revenue and maintain continuity of care.
This turnaround didn’t happen overnight, but the results speak for themselves. Here’s how Boston Senior Home Care partnered with AAFCPAs to automate their authorization process and create a replicable model that’s catching attention across Massachusetts.
Client Background & Authorization Management Challenges
Boston Senior Home Care is a private nonprofit providing home care, case management, and long-term services that support individuals in remaining in their communities. As one of Massachusetts’ 24 Aging Services Access Points (ASAPs), the organization manages a high volume of service authorizations across multiple insurance providers.
Historically, authorizations were received only in paper and PDF formats, requiring staff to manually review hundreds of documents to identify approved units and expiration dates. Without structured data or reporting, visibility was limited, increasing the risk of services being delivered without valid authorization and contributing to claim denials and lost revenue. “We had no systematic way to track or manage authorizations beyond static PDFs,” said Margaret Hogan, Chief Executive Officer of Boston Senior Home Care.
The Challenge: Managing High-Volume Insurance Authorizations in Home Care
700+ Monthly Authorizations — and No Way to Track Them
Boston Senior Home Care faced several operational constraints that limited efficiency and created financial risk. Each month, the organization received roughly 700 authorizations, most of which were in PDF format. Staff members could only process a quarter of these on time due to the sheer volume and the manual nature of the work. Without a reporting mechanism, it was difficult to track expiring or incomplete authorizations, and services were sometimes provided without proper approval.
The Cost of Inaction: $65,000 in Monthly Denials
On top of inconvenience and inefficiency, financial stakes were significant. Claim denials averaged $65,000 per month, and the organization carried nearly $1 million in long-term bad debt. Manual processes placed additional strain on staff, who were often blamed for delays beyond their control. “Imagine trying to manage the flutter of thousands and thousands of PDFs every month,” Margaret continued, describing the daily challenges faced by case managers. “It was overwhelming, and there was no practical way to track what was approved or missing.”
The organization knew opportunities existed to reduce risk, preserve revenue, and improve operations. They reached out to AAFCPAs, who recommended automating authorization processing and consolidating data into a centralized system to improve visibility, allow proactive management of approvals, and free staff to focus on client care.
The Solution: AI-Powered Authorization Automation
Working with AAFCPAs, Boston Senior Home Care implemented an end-to-end automation solution that combined AI, database management, and a dashboard to manage service authorizations more efficiently. A dedicated email address was created to receive forwarded authorization emails, which triggered the automation process. AI then extracted data from PDFs and email content, handling both structured and semi-structured formats, and populated a centralized SQL Server database, a database management system designed to store, retrieve, and manage data efficiently. This database now serves as a single repository for all authorization details, enabling consistent tracking and reporting.
The system was integrated with a Microsoft Power BI dashboard to provide real-time visualization of authorization status. This provides staff with visibility into expiring approvals, incomplete authorizations, and pending renewals at a glance, with color-coded alerts highlighting items that require immediate attention. Filters help the team prioritize workloads and act proactively rather than reacting to missed deadlines. Additionally, the SQL Server database communicates with the WellSky Aging and Disability Database (formerly known as SAMS) system to validate client eligibility, ensuring comprehensive oversight across multiple platforms.
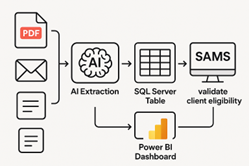
This diagram illustrates how authorization emails and PDFs move through the automation process, with AI extracting key data, SQL server storing the information, Power BI presenting it in dashboards, and the SAMS system validating client eligibility.
“Now we can monitor everything, what’s expiring, what’s missing a signature—and run comprehensive reports on authorizations,” said Margaret Hogan, Chief Executive Officer. “That visibility has been a game changer for us.”
The Results: Fewer Denials, Stronger Oversight
AAFCPAs transformed how Boston Senior Home Care manages service authorizations with a customized automation solution. The system now automatically processes 100 percent of authorization emails from participating insurers, compared with just 25 percent previously handled manually. Staff are now free of mundane, repetitive tasks and can devote more time to direct client care and proactive follow-up, boosting both efficiency and morale.
Post implementation financial results were also substantial. Specifically, monthly claim denials dropped from $65,000 to $6,000, producing a clear return on their implementation cost. By reducing denied claims and preventing revenue leakage, the organization strengthened its financial position while minimizing the risk of bad debt. Hogan described the improvement as significant, noting, “When you see how much revenue we stopped from slipping through the cracks, the return is clear—and ongoing. It is not just about recovering money we were losing. It is about giving our staff the tools to manage authorizations reliably and proactively. I’ve recommended this approach to other ASAPs because it works.”
Financial Impact Over Time
In addition to revenue recovery, operational oversight also improved. The new dashboard provides staff with visibility into expiring or incomplete authorizations, allowing them to address issues before they affect reimbursements. Enhanced reporting reduces compliance risk, ensuring all services delivered are properly authorized and documented. At the payer level, results were also measurable. For one Senior Care Options plan, Boston Senior Home Care reduced its claims denial rate from 11 percent to 1.8 percent following implementation.
What This Means for ASAPs and Healthcare Organizations
Boston Senior Home Care’s transformation demonstrates what becomes possible when ASAPs embrace intelligent automation. The results—90 percent reduction in claim denials, $59,000 in monthly savings, and staff finally freed from administrative overwhelm—represent more than operational improvements. They signal a fundamental shift toward sustainable, client-focused care delivery.
This isn’t a one-off success story. The same pressures Boston Senior Home Care faced—overwhelming PDF volumes, manual tracking systems, and staff stretched beyond capacity—challenge ASAPs nationwide. Yet their solution proves these obstacles aren’t inevitable. The combination of robotic process automation, AI, and business intelligence creates a replicable framework that can be adapted to any organization’s specific authorization workflows and payer requirements.
The question for leadership teams becomes clear: How long will you accept $65,000 monthly losses and staff burnout when proven alternatives exist? Boston Senior Home Care’s partnership with AAFCPAs created a roadmap that transforms authorization chaos into competitive advantage.
Live Client Webinar: Reduce Claim Denials
Join AAFCPAs and Boston Senior Home Care for a live client webinar demonstrating how intelligent automation reduced monthly claim denials by 90%, improved operational visibility, and strengthened financial performance.
A Path Forward for ASAP Leadership
For ASAPs ready to move beyond crisis management, the path forward starts with a single conversation about what automation could mean for your organization’s financial health and your team’s daily experience.
“It really made an enormous difference for our organization. Monthly claim denials fell from $65,000 to $6,000. The system helps us manage approvals efficiently, reduce risk, and focus on serving our clients,” said Margaret Hogan, Chief Executive Officer.
Optimize Your Business Processes for Measurable Success
Integrating the transformative power of Automation and Data Analytics, AAFCPAs provides a unique competitive advantage to our clients by embedding the strategic insights and financial acumen of experienced consulting CFOs directly into our practice. This approach ensures that our solutions not only leverage the latest in technology but are also finely tuned to the nuanced needs of finance functions and strategic financial leadership.

Vassilis Kontoglis

Charles Webb
Partner with AAFCPAs today and let our proven expertise drive your company’s growth and efficiency. Contact us now to get started!
